By Tyler Joynt, San Diego, California
As a kid, I really only knew three things about cystinosis. Doctors, sickness, and the San Diego Zoo. From an early age I remember throwing up often, going to the ER regularly, and seeing doctors frequently. I was lucky enough to be diagnosed before I was two years old, but after cysteamine had been discovered. Living in Alabama, I had access to one of the top pediatric nephrologists in the south, someone who knew cystinosis, who also happened to have a daughter that I went to school with.
Doctors’ visits to Children’s Hospital of Alabama were normal for me, and I never thought about it being weird. I took a lot of medicine around the clock, wet the bed, and vomited a lot. This was normal to me, even if it wasn’t the most fun life. My parents were very supportive and for the most part allowed me to be a regular kid. That’s where the San Diego Zoo comes in. For as long as I can remember, I’ve been doing studies all over the country in relation to cystinosis; NIH, UCSD, Stanford, Mass Gen, and others, were places I was seen and was able to travel to. I didn’t quite understand at first what I was doing. I just knew that I got to take fun trips, get poked and prodded, and talk to new doctors.
A trip we often took was to San Diego to go to UCSD to see any one of the amazing doctors there (Dr Schneider should always be remembered as THE doctor who saved us). We went so often; I believe at one point we had a seasonal pass to the zoo. If you have not been to the San Diego Zoo (or its sister, Safari Park), it is one of the most amazing experiences a kid can have and is only about 10 minutes from the UCSD Hillcrest location.
Once I was a teenager, I started to understand more about cystinosis and what these studies meant. That this disease had no cure, but doctors and researchers were working tirelessly to help give us a better life. In the mid-2000s I was “lucky” enough to be able to complete a clinical trial with Dr. Ranjan Dohil to test the first delayed-release cysteamine, or what we now know as Procysbi. It involved a tube being put down my nose and into my GI tract, where they measured my WBC (white blood cystine) cystine levels at different points of release of the medication. It wasn’t the most comfortable or fun procedure, but it was a paying study and I was able to buy myself an electric guitar.
It wasn’t until years later that I realized that the study was what brought us Procysbi, and was the first time I really saw the result of a clinical trial I had been a part of. Fast forward almost 20 years and, as God would have it, my wife and I were stationed in San Diego as a part of her military service. The gene therapy stem cell trial had begun just up the road at UCSD and after about a year of deciding not to throw my name in the hat, I decided that we’d never find the “perfect” time to do it. I was a little hesitant, but after seeing Jordan’s success I realized that I might be a great candidate and would be able to carry the torch for those unable to participate due to age, health, or location.
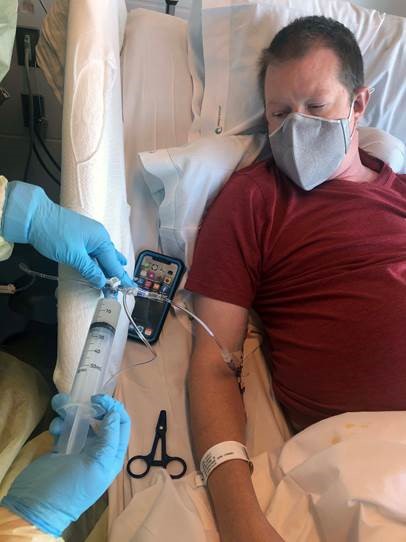
After months of preparation, a few small setbacks, and what felt like the longest day of my life, I was admitted to UCSD Jacob’s Hospital to begin the stem cell transplant on November 9, 2021. I had four days of twice-a-day chemo, 10cc of stem cells, and 22 days later, I was back home recovering. Cystinosis has been a part of my life for over 30 years, and we have come such a long way thanks to the doctors, researchers, nurses, coordinators, parents, and of course Nancy, Jeff, and Natalie Stack. I am ecstatic to have been able to have done this clinical trial for a cure, and have so much hope for a long and healthy life for today’s children (and parents) of cystinosis.